Nucor Steel, a Fortune 300 company and the largest manufacturer of recycled steel in the United States, embodies a culture that can be summarized by a decentralized management philosophy, performance-based compensation, customer service and quality, technical leadership and egalitarian benefits.
Nucor's profit sharing, scholarship program, employee stock purchase plan, extraordinary bonus and service awards are not available to the company's officers, but only to lower-level employees. Nucor is not unlike other manufacturing companies, which believe employees are a company's biggest asset.
Unlike many other companies, Nucor awards its employees for productivity and performance. That's why the idea of having onsite healthcare clinics appeals to Nucor. Safety is paramount in a steel mill. Occupational health and safety resources that enable employees to return to work promptly are built into the corporate culture at all Nucor Steel locations.
Dr. Joseph Thomas, medical officer for Nucor SC, has practiced family medicine for 20 years and emergency medicine for 10 years before transitioning to full-time onsite medicine. He now works exclusively for Nucor South Carolina, the original steel mill that Nucor built in 1965, alongside his wife, Joyce Thomas, who is a Registered Nurse for the center.
"When we built the Darlington Family Medical Center, our ultimate goal was to provide quality medical services to our team members and their families to improve their over-all wellness, prevent catastrophic illnesses and reduce overall costs for both Nucor corporate and our Nucor families. That is still our goal today," said Dr. Thomas.
One of the greatest threats to that goal through the years has been the company's obesity epidemic. "We faced a significant employee health challenge," said Dr. Thomas. "Eighty-three percent of our workforce was classified as overweight with 41 percent of that total qualifying as obese."
The average BMI at Nucor Darlington was 35; a BMI of 30 is defined as obese. Additional risk factors related to those employees with obesity include depression, diabetes, fatigue, hyperlipidemia, hypertension, joint pain, liver dysfunction, metabolic syndrome, osteoarthritis, pre-diabetes, and sleep apnea. The higher the BMI, the more risk factors an employee was found to have. Because of this, Nucor felt the negative impact of employee obesity in both direct medical costs and in employee productivity.
"The bottom line of what this is costing Nucor is important," said Dr. Thomas. "But, honestly, employee productivity is much more important to us. If employees are out because they are sick and not working1 in the mill, we are losing valuable production time. Healthy employees are happy employees; they have more energy and are more productive."
Onsite wellness began in 2006 at Nucor Berkeley when the general manager, Ladd Hall, and Dr. Thomas collaborated on wellness exams onsite. They saw that only 85 of its 900 employees had sought routine annual physicals. In the first nine months after implementing the onsite program, more than 350 employees took advantage of the wellness exams.
They knew they were onto something. The convenience of primary care had a significant impact on employee engagement and health outcomes. The company's wellness program was launched at the Darlington location in 2008 when Dr. Thomas and Joyce opened the Darlington Family Medical Center. To tackle the employee obesity issues, they started holding many "Biggest Loser" weight-loss type competitions.
Unfortunately, the participants always gained the weight back and, in many cases, gained more weight than they originally lost. "It makes sense now why that type of approach wasn't effective," said Dr. Thomas. "Weight-loss competitions are useful in generating awareness, but they lack the substantive behavioral component for long-term outcomes. As the primary care provider for employees and their families, I felt it was important to find a structured program that was easy to follow and addressed behavioral challenges to not only help them lose weight, but keep it off."
After a great deal of research, Dr. Thomas and Joyce discovered a program that offered a behavioral approach to obesity management that was proven to have clinical effectiveness. Outcomes of its effectiveness were published in the American Journal of Medicine.Upon further research, Dr. Thomas and Joyce learned that a one-year study abstract reported 95 percent of the patients who had seen their provider after 12 months had maintained their weight loss.2
The program's data outcomes impressed Nucor, but as many healthcare providers know, treating obesity is complex and not something learned in medical school. Implementing the program within the Darlington Family Medical Center needed to be considered. As it happens, the company offering the clinical program had developed software that automated much of the "heavy lifting" of obesity management.
PondusHealth (with its sister company The Center for Medical Weight Loss) had created a software platform that incorporated more than 10 years of obesity care learnings from among hundreds of independent physicians and nurse practitioners in the United States.
The platform is called ObesityTx. PondusHealth also offered a robust ROI model that helped Dr. Thomas build the business case to show Nucor's medical cost and productivity savings. Dr. Thomas considers the tool a great resource to help Nucor track its ongoing costs and savings.
"Data is crucial to measuring our performance. I don't know many vendors that step up to the plate and provide ongoing data like they do," said Dr. Thomas.
THE PROCESS
A primary goal of PondusHealth was to make the installation process as easy as possible for Nucor/Darlington Family Medical Center. The ObesityTx platform, which provides predictive weight-loss algorithms and web-based automated personalized obesity behavioral counseling plans, required just three pieces of equipment - a body composition analysis (BCA) scale, a laptop, and a printer.
Dr. Thomas' team did not have to invest a lot of time learning the system because of the technical integration of the devices and automation built into the software.In addition to system training, Dr.Thomas and his staff needed to complete clinical training in obesity medicine before they could officially launch the medical weight-loss behavior program.
PondusHealth offers both live and online program training, so it is flexible for those that cannot get out of their office for face-to-face training. Once Dr. Thomas and his staff were ready, they worked with the vendor to develop a communication strategy to invite the 628 eligible Nucor employees and dependents to sign up. Pondus Health provided all the graphics and help necessary to customize the right message.
Nucor used its internal TV monitors, flyers, posters and a personal invitation from Dr. Thomas in the monthly email newsletter he sends to employees. The response was overwhelming: 187 signed up immediately; 84 were put on the waiting list. "We are adding new participants on a regular basis," said Dr. Thomas.

Nucor fully subsidized each participating employee and dependent for the first 12 weeks, which consisted of personalized behavioral counseling sessions and a controlled calorie meal plan. Employees who continued past the initial 12 weeks paid out-of-pocket for meal items, but behavioral counseling visits remained fully subsidized.
All services at the Darlington Family Medical Center are free including prescriptions from on-site medication dispensing, take-home sleep units for studies and chiropractic services. PondusHealth's ObesityTx system also provides patients access to all program data via smart phone, tablet, or laptop to stay connected and engaged - a key component to sustaining weight-loss.
"Adding a tablet for the patients to complete their behavioral questionnaires and counseling modules in the office lobby if they didn't prior to the visit comes in handy," said Joyce Thomas.To date, more than 5,000 pounds have been lost and 158 participants have been screened.
OBESITY: CHRONIC DISEASE
In 2012, the U.S. Preventative Services Task Force recommended all primary care physicians screen their adult patients for obesity and patients with a body mass index (BMI) of 30 kg/m2 or higher be offered or referred to intensive multicomponent behavioral interventions.3
In 2013, the American Medical Association confirmed obesity as a chronic disease and should be treated with the chronic care model.4 Dr. Thomas agrees and isscreening all of his employee patients and their dependents following the chronic care model and offering customized behavioral counseling with his medical weight-loss program to help Nucor employees and dependents change their habits.
MEASURING RESULTS - DATA IS CRUCIAL
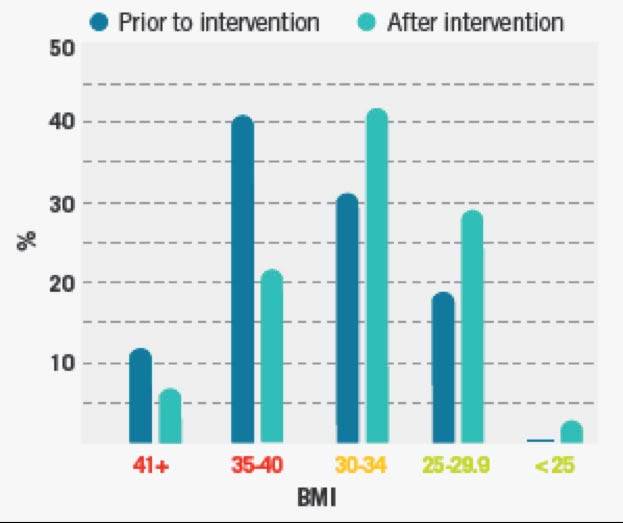
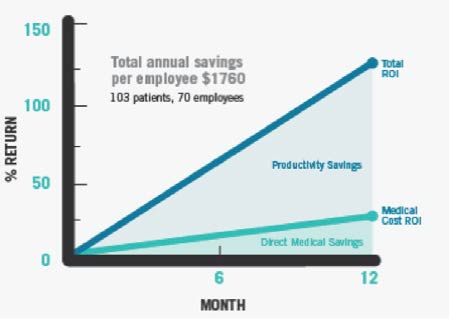
"In addition to BMI, we identified our eligible employee participants by taking a look at their health-risk factors,such as blood pressure, cholesterol and blood-sugar levels," said Dr. Thomas. The charts below show how the employees' BMI improved after the intervention and the positive ROI Nucor received in Year One.
The highest risk employee population was reduced by 43 percent. The total annual savings per employee was $1,760. Dr. Thomas also reported that several employees and dependents reduced or eliminated medications to treat comorbid conditions, such as Type 2 Diabetes.-- Highest risk employee population reduced by 43 percent;-- ROI is positive in Year 1;-- ObesityTx system continues ongoing data collection.
NUCOR EMPLOYEES
Dawn Thompson - "Having the medical weight-loss program right at the clinic makes it so convenient. We work 12-hour shifts. If it wasn't onsite, I wouldn't have done it. Joyce helped me learn how to eat, shop and cook in a healthy way. My husband tells me every day how sexy I am."Jeffrey Johnson - "This is one of the best things I have ever done other than my children being born. It has completely changed my life! You have to stay connected to the clinic and come back regularly so you can stay on track after you lose your weight.
Keeping it off is the most important thing. "Today, many large corporations are exploring different provider-based approaches to obesity management, such as company-owned onsite clinics, contracting with third- party clinic administrators, partnering with a local hospital system, or a blend of those models. The company-owned, on-site primary care clinic model works extremely well within the Nucor culture.
Dr. Thomas readily admits he is personally and professionally committed to helping both his patients and the company. He loves what he does and takes a great deal of pride when he sees his Nucor family achieve its goals. "This program has led to a lot of happy employees who have a renewed level of productivity," said Dr. Thomas.
"It also will save more money than anything else we do in the long run. It's been so successful that we hope to have a 900-square foot building dedicated to the weight-loss program, at some point in the near future."

Sources
1. Hass, W. C.; Moore, J. B.; Kaplan, M.; Lazorick, S.; "Outcomes from a Medical Weight-Loss Study"; The American Journal of Medicine; 2012; Vol. 125, 603.e7-603.
2. Claim: 95.3 percent of patients were at a lower weight in one year. Based on original sample of 550 obese men and women who began a CMWL program, 150 original patients continued care for 12 months and visited physician in 12th month of care.
3. U.S. Preventative Services Task Force Announcement; Sept. 4, 2012; Annals of Internal Medicine; Vol. 157, No. 5.
4. "Obesity is a Chronic Disease"; American Medical Association; Full Resolution; http://www.npr.org/documents/2013/jun/ama-resolution-obesity.pdf; Accessed May 19, 2015.








